Healthcare Claim Management Market Size and Share
Healthcare Claim Management Market Analysis by Mordor Intelligence
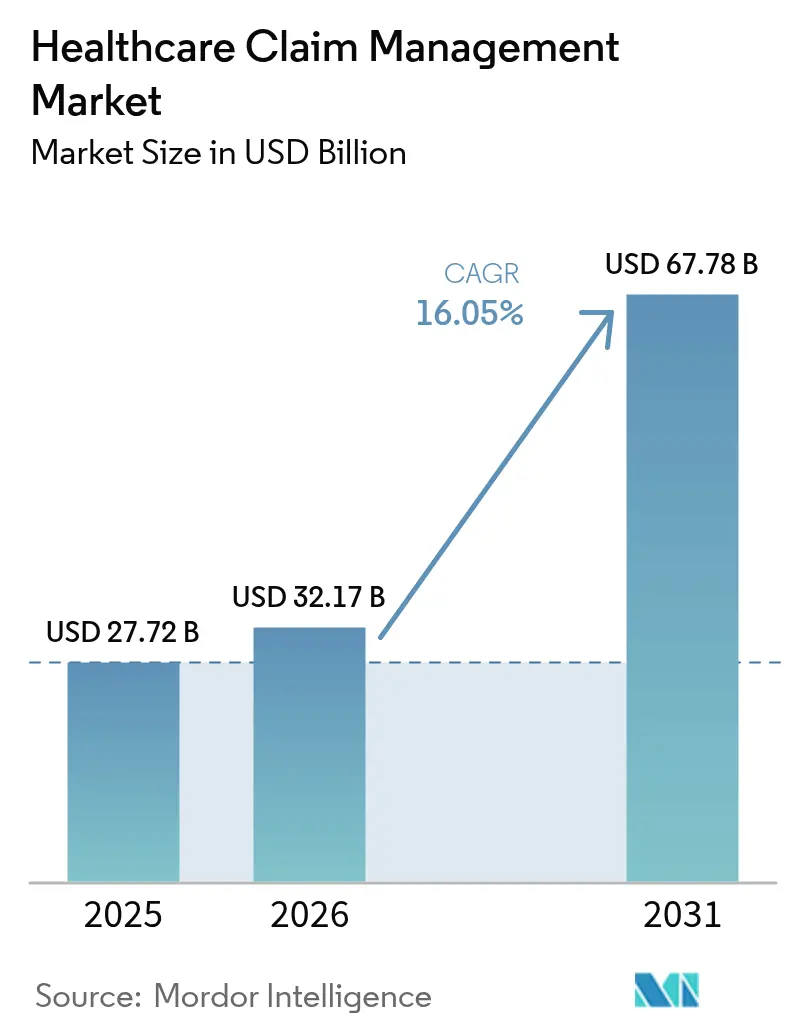
The healthcare claims management market size was valued at USD 27.72 billion in 2025 and estimated to grow from USD 32.17 billion in 2026 to reach USD 67.78 billion by 2031, at a CAGR of 16.05% during the forecast period (2026-2031). Rapid digitalization, rising claim-denial expenses, and mounting pressure to improve payment accuracy encourage payers and providers to replace manual workflows with AI-driven platforms. Hospitals now spend USD 19.7 billion annually overturning denied claims, underscoring the urgency for automation. Cloud deployment gains momentum as organizations favor real-time analytics at scale, while integrated revenue-cycle suites and payment-integrity modules converge to minimize revenue leakage. Moderate consolidation continues as established vendors acquire niche innovators to accelerate time-to-market for generative AI tools that offset an expected 100,000-worker shortfall in healthcare administration by 2028[1]American Hospital Association, “Hospital Denial Recovery Report 2025,” aha.org.
Key Report Takeaways
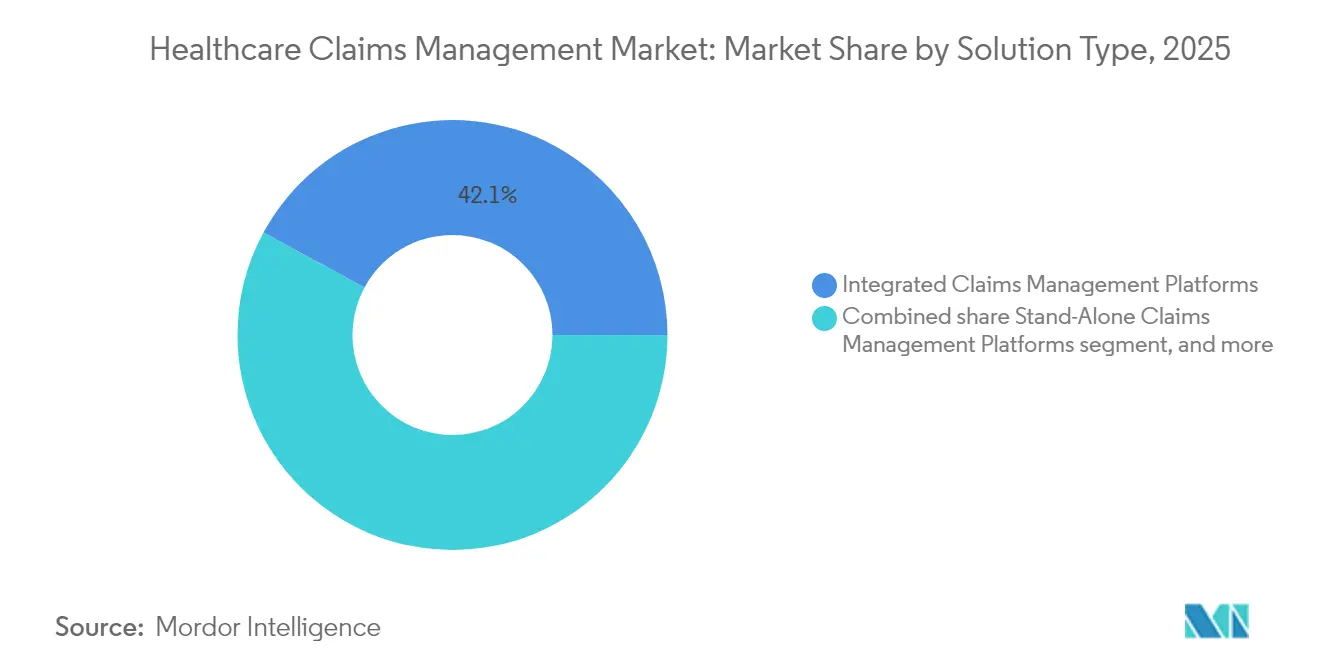
- By solution type, integrated claims-and-RCM suites led with 42.10% revenue share in 2025, whereas AI-based denial-management modules are projected to expand at an 18.21% CAGR through 2031.
- By component, software accounted for 62.65% of spending in 2025; services are pacing ahead with a 9.85% CAGR to 2031 as providers seek implementation and managed-services support.
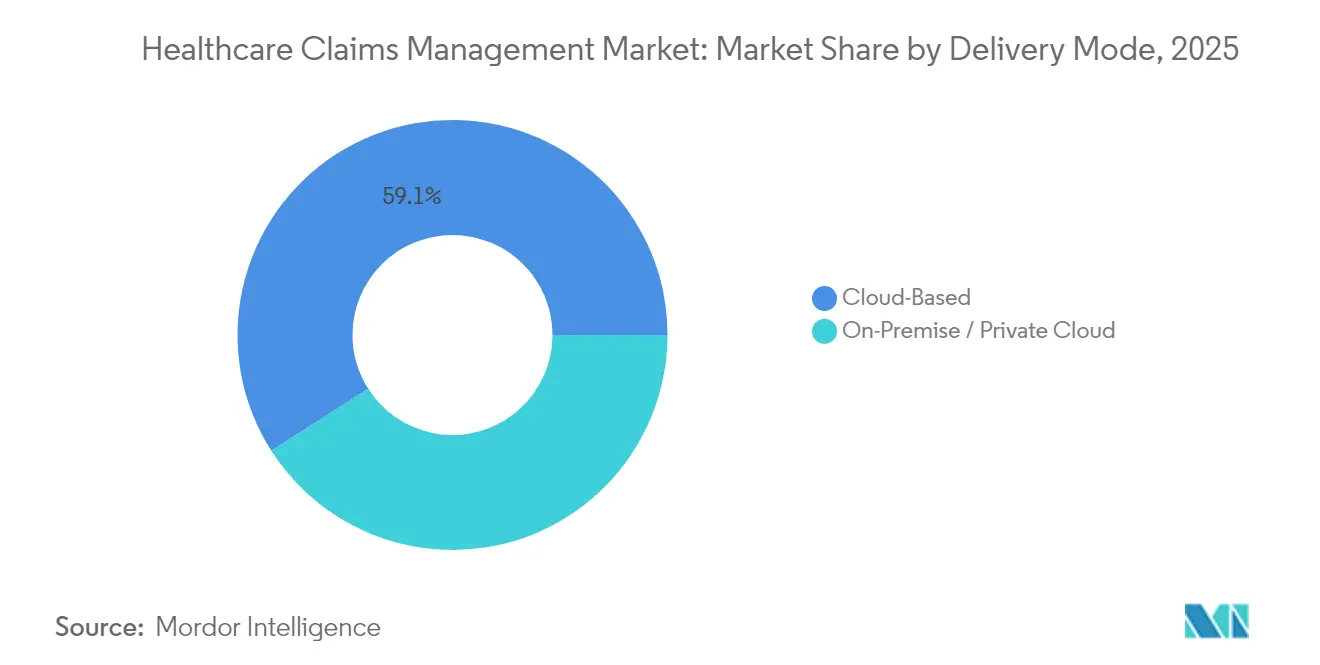
- By delivery mode, cloud deployments captured 59.05% of the healthcare claims management market size in 2025 and are growing at an 18.40% CAGR thanks to scalability and rapid data-exchange capabilities.
- By end-user, payers processed 53.70% of claims volume in 2025, while third-party administrators recorded the fastest 19.15% CAGR as self-funded employers outsource benefit administration.
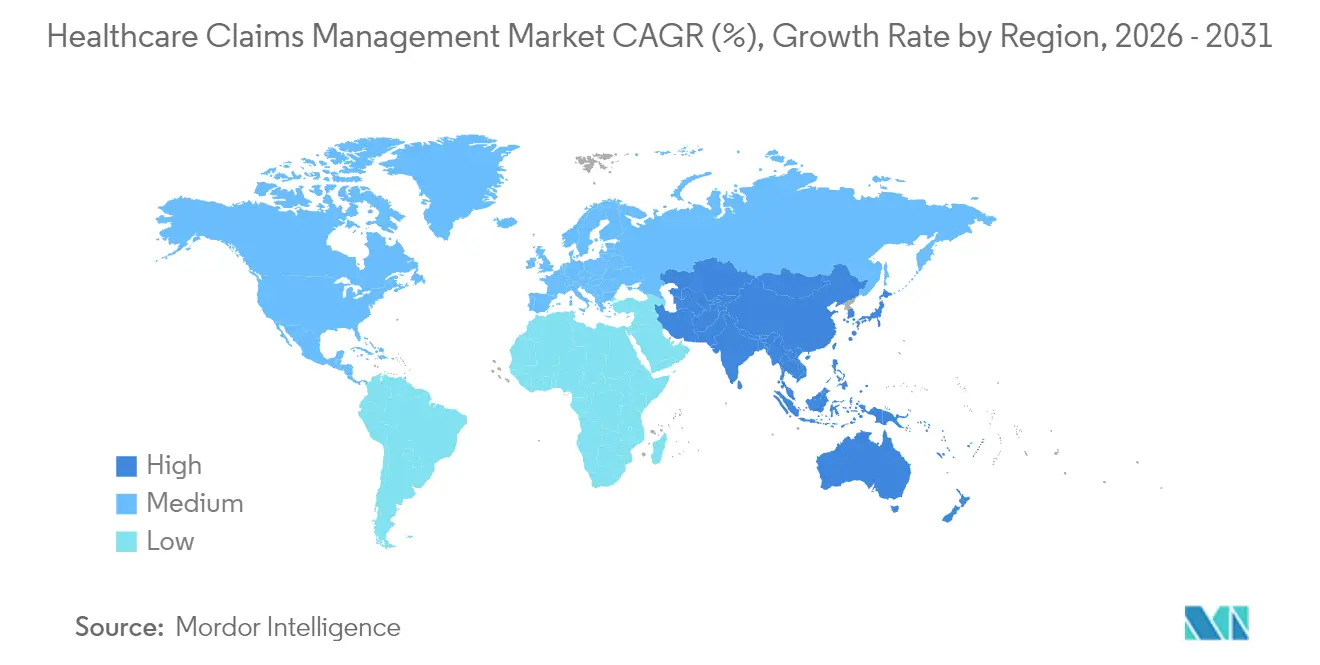
- By geography, North America retained 45.90% of 2025 revenue; Asia-Pacific is the fastest-growing region with a 17.20% CAGR to 2031, driven by expanding insurance coverage and digital-health investment.
Note: Market size and forecast figures in this report are generated using Mordor Intelligence’s proprietary estimation framework, updated with the latest available data and insights as of 2026.
Global Healthcare Claim Management Market Trends and Insights
Driver Impact Analysis*
| Driver | % Impact on CAGR Forecast | Geographic Relevance | Impact Timeline |
|---|---|---|---|
| Expansion of public and private health-insurance coverage | +2.8% | Global; early gains in Asia-Pacific | Medium term (2-4 years) |
| Escalating financial impact of claim denials | +3.2% | North America and EU; spill-over to APAC | Short term (≤2 years) |
| Growing geriatric and chronic disease population | +2.1% | Global; concentrated in developed markets | Long term (≥4 years) |
| Adoption of AI-enabled payment-integrity platforms | +4.1% | North America core, expanding to APAC and EU | Short term (≤2 years) |
| Deployment of robotic process automation in claims adjudication | +2.9% | Global; enterprise-level early adoption | Medium term (2-4 years) |
| Shift toward value-based and real-time reimbursement models | +1.4% | North America lead; gradual APAC adoption | Long term (≥4 years) |
| Source: Mordor Intelligence | |||
Expansion Of Public and Private Health-Insurance Coverage
Wider insurance adoption adds millions of newly covered lives, increasing claims volume and complexity. Emerging Asia-Pacific markets accelerate digital reforms, illustrated by Thailand’s AI-enabled universal-coverage roadmap and India’s push to integrate national health records with payer systems. In the United States, the Medicare Shared Savings Program continues to migrate providers into accountable-care contracts, driving demand for analytics-rich platforms that reconcile shared-savings payments[2]Centers for Medicare & Medicaid Services, “National Health Care Spending Update 2025,” cms.gov.
Escalating Financial Impact of Claim Denials
Denial rates reached 11.8% in 2024, costing hospitals USD 19.7 billion in rework and lost revenue. The average denied claim costs USD 25–181 to remediate, and 65% of denied cases are never resubmitted, making proactive denial avoidance essential. Intermountain Health used advanced analytics to recoup USD 20 million and projected USD 35 million in future savings by restructuring its denial-management workflow.
Growing Geriatric and Chronic Disease Population
An aging population raises chronic-care claims that require accurate risk adjustment and longitudinal data. Academic medical centers that embedded chronic-care coordination into claims workflows improved continuity-of-care billing accuracy, while updated risk-adjustment models reward precise capture of social-determinant codes with a 2.9% rate uplift.
Adoption Of AI-Enabled Payment Integrity Platforms
AI engines that cross-reference clinical, coding, and utilization data help payers detect overpayments, fraudulent claims, and coding errors. Optum’s CARE Rules Engine cuts manual audit hours by 4,500–5,000 annually for several state Medicaid programs. Waystar’s new generative AI tool drafts appeal letters for the 450 million denied claims processed each year, promising significant labor savings.
Restraints Impact Analysis*
| Restraints Impact Analysis | (~) % Impact on CAGR Forecast | Geographic Relevance | Impact Timeline |
|---|---|---|---|
| Stringent patient-data privacy and cybersecurity regulations | –1.8% | Global; stricter EU and North America enforcement | Short term (≤2 years) |
| High upfront implementation and migration costs | –2.3% | Global; mid-size organizations most affected | Medium term (2-4 years) |
| Interoperability challenges across legacy core systems | –1.6% | Global; concentrated in established markets | Medium term (2-4 years) |
| Shortage of analytics and AI-skilled workforce | –1.9% | Global; acute in North America and EU | Long term (≥4 years) |
| Source: Mordor Intelligence | |||
Stringent Patient Data Privacy and Cybersecurity Regulations
Global frameworks such as GDPR and HIPAA impose stiff penalties for data breaches, compelling vendors to invest in zero-trust architectures and end-to-end encryption. Frequent ransomware attacks on healthcare facilities heighten executive focus on security certifications and continuous monitoring.
High Upfront Implementation and Migration Costs
Modern platforms require API gateways, data-quality audits, and staff retraining. Mid-tier hospitals often defer digital upgrades because annual capital budgets remain flat. Subscription-based managed-service models help distribute costs over multi-year contracts, but CFOs still scrutinize return-on-investment timelines.
*Our updated forecasts treat driver/restraint impacts as directional, not additive. The revised impact forecasts reflect baseline growth, mix effects, and variable interactions.
Segment Analysis
By Solution Type: AI-Based Modules Drive Innovation
Integrated platforms dominated 2025 with a 42.10% revenue share as organizations adopted enterprise-wide suites that merge eligibility, prior authorization, and revenue-cycle tools into a single workspace. The healthcare claims management market continues to prize all-in-one ecosystems that lower vendor sprawl and simplify compliance audits. AI-based denial-management modules, however, are set to grow at an 18.21% CAGR through 2031 as administrators target denial rates above 10%. These apps mine claims, coding, and clinical notes to flag high-risk submissions before they reach payers, reducing rework costs.
Standalone payment-integrity engines remain attractive to mid-size payers that want rapid fraud-detection gains without replacing core adjudicators. Optum’s Integrity One recorded more than 20% coder-productivity gains during beta testing, while one regional health plan using Cognizant’s analytics stack cut pending inventory fifteen-fold. The healthcare claims management market therefore shows a clear pivot from retrospective auditing to concurrent and prospective risk scoring.

By Component: Services Segment Accelerates
Software licenses represented 62.65% of 2025 spending, reflecting large investments in AI rule sets, API libraries, and workflow orchestration engines that anchor modern platforms. Yet the services category is advancing at a 9.85% CAGR as hospitals, payers, and TPAs contract for implementation, configuration, and ongoing optimization support. Outsourced claims-processing units fill critical labor gaps, and managed-service deals guarantee SLAs that internal teams struggle to match.
Consulting engagements often revolve around privacy-impact assessments, TEFCA readiness, and value-based-contract modeling. As legacy COBOL systems sunset, providers rely on service partners to migrate millions of records without downtime. Consequently, the healthcare claims management market size for advisory and managed-services lines is forecast to outpace license revenue growth over the next five years.
By Delivery Mode: Cloud-Based Solutions Dominate Growth
Cloud deployments held 59.05% revenue in 2025 and are outpacing overall market growth at an 18.40% CAGR as enterprises favor elastic storage and always-on analytics. Florida Blue’s claims modernization achieved a 40% processing-speed improvement after refactoring micro-services in a secure public-cloud tenancy that scales on demand. The healthcare claims management market share of on-premise systems continues to shrink as CIOs prioritize disaster-recovery resilience and pay-per-use economics.
Institutions with strict data-residency requirements still choose hybrid models, retaining sensitive PHI on private clouds while using public compute pools for model training. Anthem’s collaboration with IBM and Amazon Web Services processes 750 million claims annually and reduced high-priority incidents 25% within one year IBM. Blockchain pilots that trace claim edits across stakeholders also favor cloud-native stacks, further strengthening the deployment shift.

By End-User: TPAs Experience Rapid Expansion
Payers managed 53.70% of total claims in 2025, leveraging in-house adjudication engines and nationwide provider networks. Yet TPAs display the fastest 19.15% CAGR as self-funded employers seek flexible benefit designs and transparent fee models. The global TPA sector topped USD 488.9 billion in 2024 and continues to migrate toward AI-enabled automation that slashes overhead.
Hospitals deepen investment in purpose-built denial-management portals to recoup lost revenue, while large physician groups deploy real-time eligibility checks to support value-based contracts. Employers working with TPAs demand dashboards that expose cost trends, prompting administrators to embed predictive analytics that flag high-cost members for early intervention. As a result, the healthcare claims management market size tied to employer-sponsored plans expands steadily through 2030.
Geography Analysis
North America accounted for 45.90% of 2025 revenue, underpinned by Medicare, Medicaid, and commercial insurers that together adjudicate billions of claims annually. Federal mandates such as the 21st Century Cures Act and TEFCA enforce FHIR interoperability, prompting continuous platform upgrades. Canada’s single-payer model drives provincial initiatives to automate eligibility verification, while Mexico’s insurance-expansion programs fuel new deployments among social-security institutes.
Asia-Pacific is the fastest-growing region with a 17.20% CAGR, propelled by compulsory insurance schemes, rapid private-payer expansion, and governmental AI roadmaps. China encourages AI-based claim verification within its national-reimbursement-drug list to curb fraud, and Japan embraces chronic-care registries to manage an expanding elder population. India integrates health-identity numbers with payer databases to streamline e-claims, and Australia’s shared health-record platform accelerates real-time adjudication for tele-consults.
Europe maintains steady adoption as GDPR compliance and e-prescription mandates shape purchasing priorities. Germany promotes semantic interoperability standards in the Krankenhauszukunftsgesetz funding program, while the United Kingdom’s NHS upgrades spine services to support centralized prior-authorization workflows. Southern European countries invest European Recovery funds to modernize claims portals that enable cross-border treatment billing. Collectively, these initiatives ensure the healthcare claims management market continues its expansion across the continent.
Competitive Landscape
Market concentration is moderate. Optum anchors the top tier by coupling claims platforms with analytics, network management, and payment-integrity services. New Mountain Capital and KKR continue multi-billion-dollar roll-ups to assemble scaled payment-accuracy portfolios that compete on breadth of AI models. Oracle previewed an EHR-native claims module that merges clinical and financial data, signaling a trend toward one-stop platforms.
Technology differentiation now rests on generative AI. Waystar’s AltitudeCreate automatically drafts appeal letters and integrates with Epic work queues, reducing staff workload and cycle times. Cognizant delivered 92% adjudication-cost savings for one large payer by orchestrating RPA bots across eligibility, price checking, and compliance edits.
White-space opportunities persist in mid-market hospitals that need turnkey SaaS offerings, in niche modules addressing social-determinant coding, and in real-time enrichment APIs for value-based care scorecards. Vendors that guarantee zero-trust security and low-code configuration stand to gain share as chief information security officers and clinical executives jointly evaluate new purchases. The anticipated administrative-talent shortfall further incentivizes product roadmaps that embed self-service analytics and conversational AI helpers.
Healthcare Claim Management Industry Leaders
Optum, Inc.
Mckesson Corporation
Cognizant (Trizetto)
Oracle
Accenture Plc
- *Disclaimer: Major Players sorted in no particular order


Recent Industry Developments
- April 2025: Transcarent completed a USD 621 million merger with Accolade, creating an advocacy platform serving more than 20 million members with AI-powered navigation, pharmacy, and oncology services.
- April 2025: Centauri Health Solutions acquired MedAllies, adding secure-messaging and data-exchange capabilities used by 1,000 hospitals and 125,000 clinicians.
- March 2025: Optum launched Integrity One, an AI-based revenue-cycle platform that raised coder productivity by 20% during pilot implementations.
- February 2025: Commure and Athelas signed a definitive agreement to buy Augmedix, aiming to automate 80% of denied-claim resubmissions across more than 3 million annual physician visits.
- February 2025: Teladoc Health acquired Catapult Health for USD 65 million, expanding at-home wellness exams and early-detection analytics to roughly 3 million covered lives.
Research Methodology Framework and Report Scope
Market Definitions and Key Coverage
Our study defines the healthcare claims management market as all software and related managed or consulting services that automate claim intake, adjudication, denial management, payment integrity, and analytics for public or private payers, providers, and third-party administrators across inpatient, outpatient, and ancillary settings.
Scope Exclusions: Pure property and casualty, workers' compensation, or automobile claim platforms that lack healthcare claim functionality are excluded.
Segmentation Overview
- By Solution Type
- Integrated Claims Management Platforms
- Stand-Alone Claims Management Platforms
- Ai-Based Denial Management Modules
- Payment Integrity Solutions
- By Component
- Software
- Services (Bpo, Consulting, Managed)
- By Delivery Mode
- Cloud-Based
- On-Premise / Private Cloud
- By End-User
- Healthcare Payers (Public And Private)
- Healthcare Providers
- Third-Party Administrators (Tpas)
- Geography
- North America
- United States
- Canada
- Mexico
- Europe
- Germany
- United Kingdom
- France
- Italy
- Spain
- Rest of Europe
- Asia-Pacific
- China
- Japan
- India
- Australia
- South Korea
- Rest of Asia-Pacific
- Middle East & Africa
- GCC
- South Africa
- Rest of Middle East & Africa
- South America
- Brazil
- Argentina
- Rest of South America
- North America
Detailed Research Methodology and Data Validation
Primary Research
Mordor analysts interviewed payers, large hospital revenue cycle officers, independent billing service managers, and health IT vendors across North America, Europe, and Asia-Pacific. These discussions clarified average claim handling cost, cloud adoption pace, and the real impact of AI-driven denial analytics, enabling us to filter and fine-tune secondary findings.
Desk Research
We began by mapping the addressable pool from freely available sources such as CMS National Health Expenditure tables, OECD Health Stats, WHO Global Health Observatory, and regional insurance regulator portals that publish annual claim volumes and loss ratios. Trade associations, America's Health Insurance Plans, European Health Insurance Cards, Asia-Pacific Healthcare Administrators Forum, and peer-reviewed journals on denial rates supplied additional operating benchmarks. Company 10-Ks, investor decks, and reputable business news archived on Dow Jones Factiva enriched pricing, vendor revenue splits, and recent contract awards. This list is indicative; numerous other public documents were consulted to cross-check figures and definitions.
Market Sizing and Forecasting
A top-down construct using national healthcare spending, insured population, and average claims per member set the ceiling. Results were cross-validated through selective bottom-up supplier roll-ups and sampled average selling price multiplied by installations for leading platforms. Key variables like claim denial rate, cloud penetration in RCM, AI module uptake, payer digital spending ratio, and regulatory turnaround targets drive yearly adjustments. We forecast with multivariate regression blended with scenario analysis to capture shifts in reimbursement policy and technology pricing. Where bottom-up totals diverged beyond three percent, intermediate inputs were re-benchmarked with fresh interviews before locking the baseline.
Data Validation and Update Cycle
Outputs move through variance checks, peer review, and a senior analyst sign-off. Models refresh annually, with interim updates triggered by material regulation or mega merger announcements. Before release, we perform a final parameter sweep so clients receive the most current view.
Why Mordor's Healthcare Claim Management Baseline Inspires Reliability
Published market values often differ because firms pick unique service mixes, pricing ladders, and refresh cadences. Our disciplined scoping, transparent variable choice, and yearly recalibration mean decision-makers can lean on a balanced midpoint rather than extremes.
The comparison shows that when scope breadth, timely base year selection, and multi-source validation converge, Mordor provides a dependable midpoint that stakeholders can trace back to clear metrics and repeatable steps.
Benchmark comparison
| Market Size | Anonymized source | Primary gap driver |
|---|---|---|
| USD 27.72 B (2025) | Mordor Intelligence | - |
| USD 40.77 B (2024) | Global Consultancy A | Includes broader revenue cycle modules and projects aggressive AI price inflation |
| USD 25.44 B (2022) | Industry Analyst B | Uses older base year and applies constant currency without recent claim volume surge |
| USD 16.77 B (2024) | Trade Journal C | Focuses solely on software, omits managed and consulting service revenues |
The comparison shows that when scope breadth, timely base year selection, and multi-source validation converge, Mordor provides a dependable midpoint that stakeholders can trace back to clear metrics and repeatable steps.


Key Questions Answered in the Report
What is the current size of the healthcare claims management market?
The market generated USD 32.17 billion in 2026 and is on track to reach USD 67.78 billion by 2031 at a 16.05% CAGR.
Which solution type is growing fastest?
AI-based denial-management modules hold the top growth outlook with an 18.21% CAGR through 2031 as organizations focus on preventing revenue leakage.
Why are cloud deployments becoming dominant?
Cloud platforms deliver elastic compute, real-time analytics, and stronger disaster-recovery capabilities, capturing 59.05% of 2025 spending and expanding at an 18.40% CAGR.
How do claim denials impact hospital finances?
Hospitals spend USD 19.7 billion each year overturning denied claims, and 65% of denials are never resubmitted, making proactive denial avoidance critical.
What role do third-party administrators play?
TPAs are the fastest-growing end-user segment with a 19.15% CAGR as self-funded employers outsource claims tasks and demand transparent, AI-driven analytics.
Which region is expected to see the highest growth?
Asia-Pacific leads with a projected 17.20% CAGR to 2031, driven by expanding insurance coverage and government-backed digital-health investments.
Page last updated on:









