Pharmacy Benefit Management Market Size and Share
Pharmacy Benefit Management Market Analysis by Mordor Intelligence
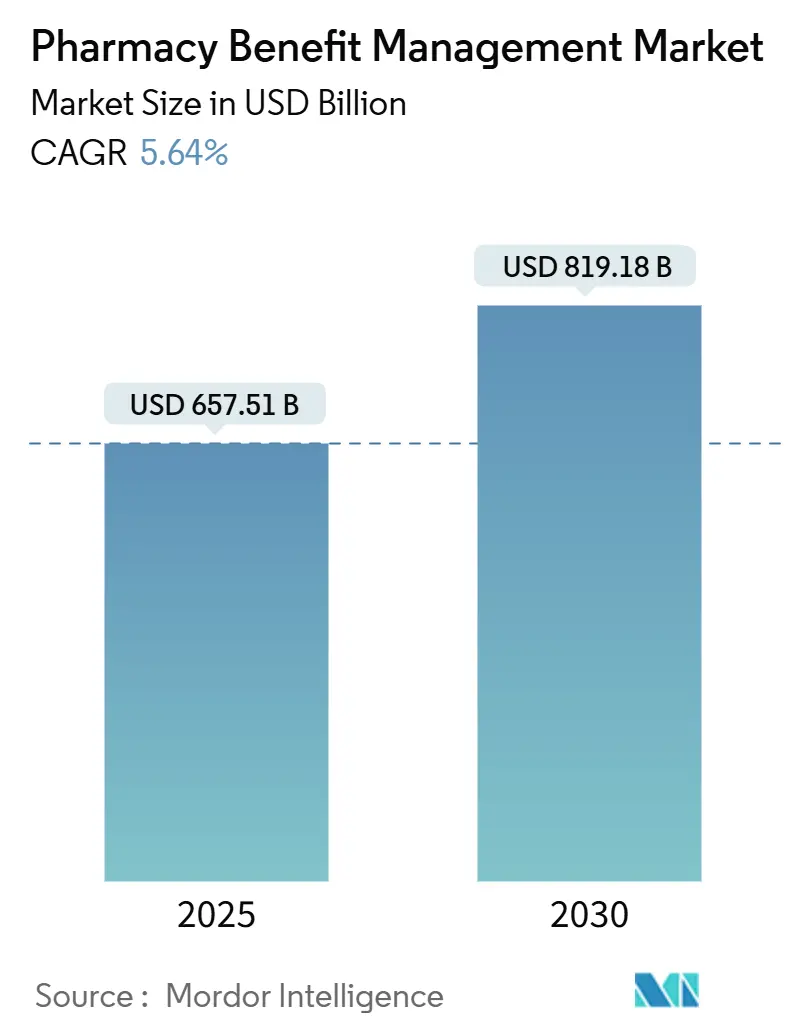
The Pharmacy Benefit Management market was valued at USD 657.51 billion in 2025 and is forecast to climb to USD 819.18 billion by 2030, advancing at a 5.6% CAGR from 2025 to 2030. Rising prescription-drug spending—now 27.0% of employer medical outlays—underscores the growing reliance on PBMs for cost control. The upswing also reflects surging specialty-drug utilization, accelerated employer scrutiny of benefit contracts, and technology investments that streamline claims and prior authorization workflows. North America leads the Pharmacy Benefit Management market with 46.3% revenue share, while Asia Pacific records the fastest growth as coverage expands in China and India. Competitive intensity remains high as vertically integrated PBMs consolidate buying power, even as transparent newcomers chip away at rebate-driven models.
Key Report Takeaways
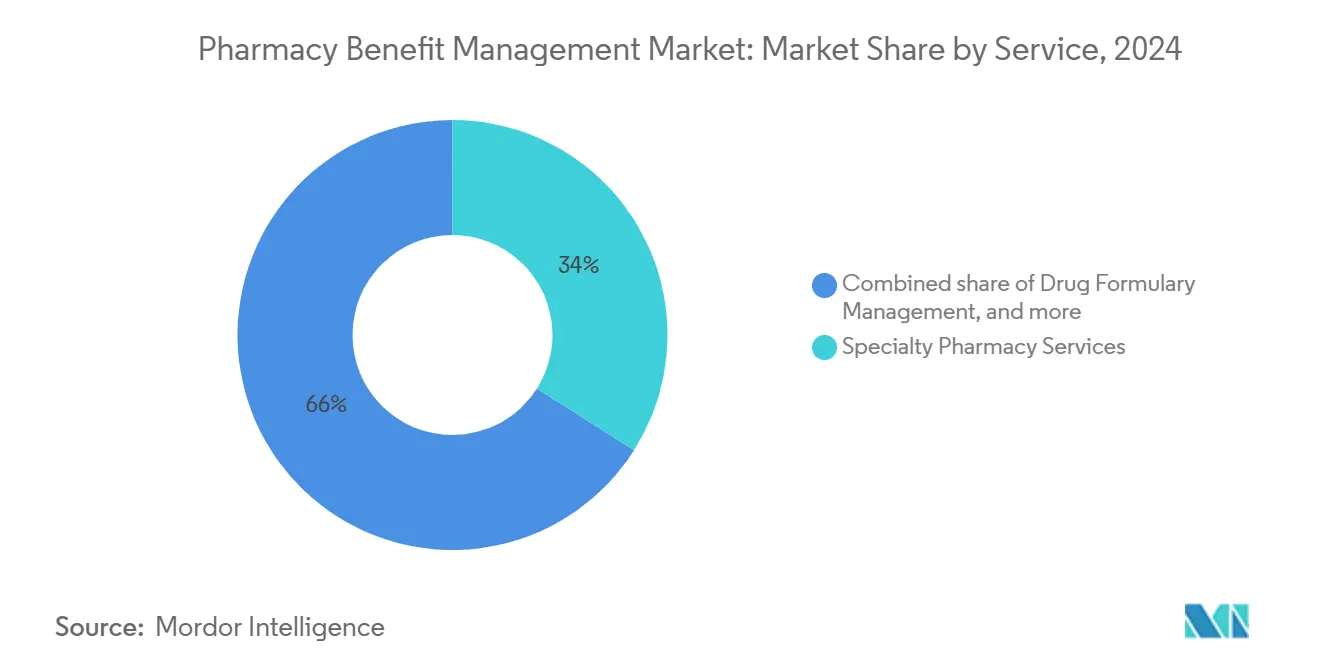
- By service, specialty pharmacy services led with 34.0% revenue share in 2024, whereas claims processing & adjudication is poised for a 7.5% CAGR through 2030.
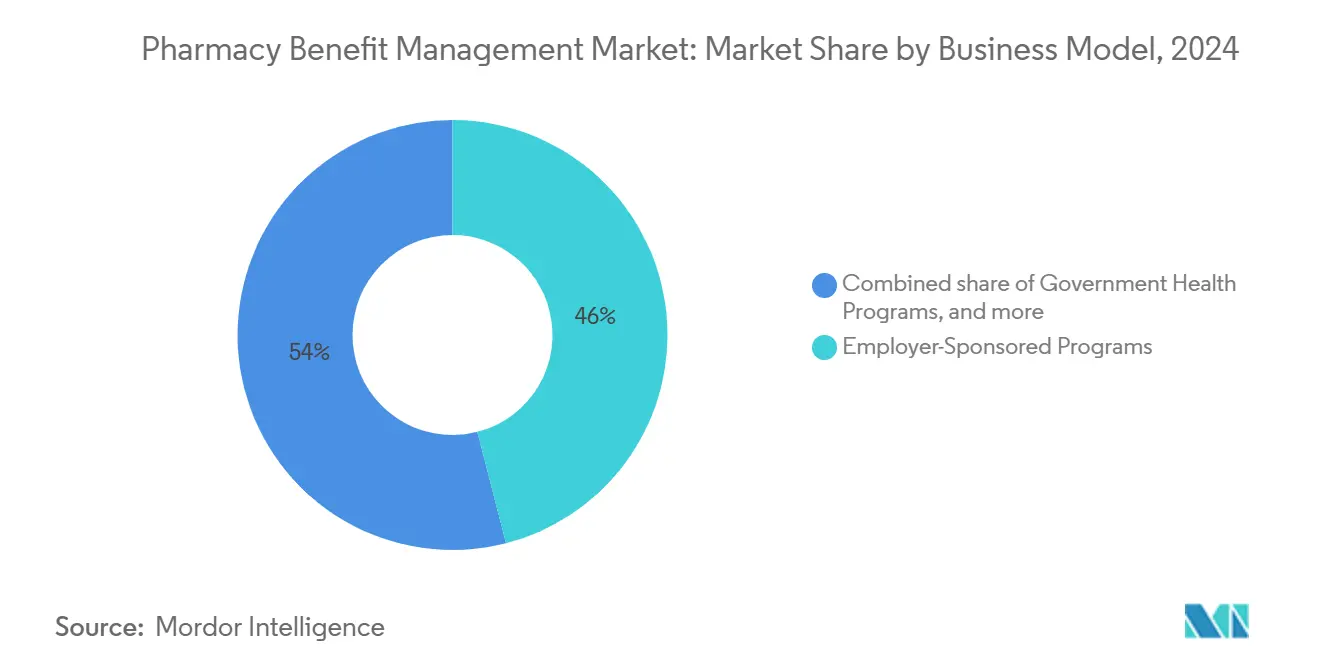
- By business model, employer-sponsored programs controlled 46.0% of the pharmacy benefit management market share in 2024; government health programs show the quickest rise at a 6.7% CAGR to 2030.
- By end user, PBM organizations and retail pharmacies jointly held 75.0% share in 2024; Mail-order pharmacies are projected to expand at an 8.2% CAGR through 2030.
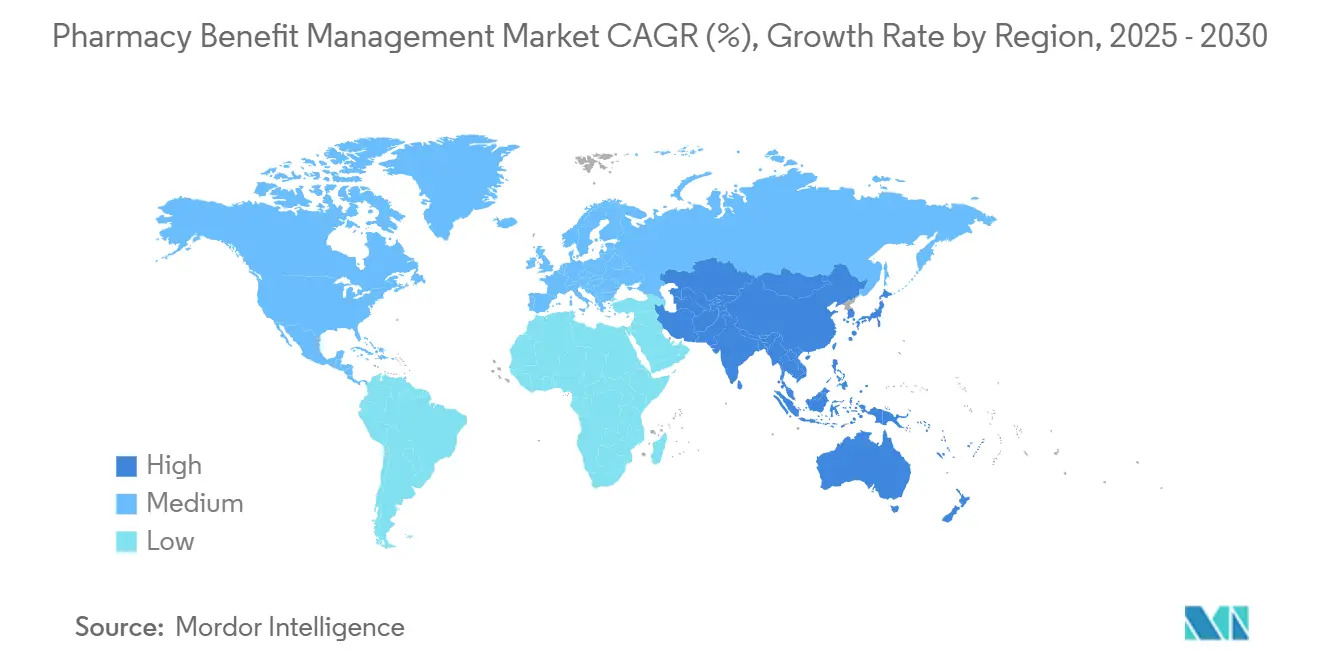
- By region, North America dominated with 46.3% in 2024, whereas Asia Pacific is expected to log a 7.6% CAGR, lifting the region to USD 147.1 billion by 2030.
Global Pharmacy Benefit Management Market Trends and Insights
Drivers Impact Analysis
| Drivers Impact Analysis | (~) % Impact on CAGR Forecast | Geographic Relevance | Impact Timeline |
|---|---|---|---|
| Escalating specialty-drug costs | +1.9% | Global | Long term (≥ 4 years) |
| Expansion of public & private coverage pools | +1.3% | North America, Asia Pacific | Medium term (2-4 years) |
| Shift to value-based pharmacy benefits | +1.1% | North America, Europe | Medium term (2-4 years) |
| Digital transformation & workflow automation | +0.9% | Global | Short term (≤ 2 years) |
| Rising demand for cost transparency & pass-through pricing models | +1.0% | North America, Europe | Short term (≤ 2 years) |
| Consolidation & vertical integration across the drug-supply chain | +0.8% | North America | Long term (≥ 4 years) |
Source: Mordor Intelligence
Escalating Prescription-Drug Expenditure & Therapeutic Complexity
Specialty medicines accounted for 54% of hospital drug spend in 2025, pressuring payers to adopt PBM models that integrate clinical expertise with utilization controls. The popularity of GLP-1 agonists for diabetes and obesity may lift that therapeutic class toward USD 100 billion within five years, requiring tighter formulary rules and step-therapy edits. Oncology pipelines and orphan drugs compound complexity, while multimorbidity drives polypharmacy across age cohorts. PBMs deploying advanced analytics can coordinate regimens, flag duplication, and negotiate indication-based contracting that balances outcomes with affordability. These pressures support sustained demand for Pharmacy Benefit Management market solutions through 2030.
Expansion of Public & Private Health-Coverage Pools
Medicare Part D is forecast to reach 36% of U.S. drug spending by 2032, up from 2024 levels. The Inflation Reduction Act caps out-of-pocket Part D costs at USD 2,000 for 18.7 million members beginning in 2025. Commercial employers are simultaneously re-bidding contracts, with 52% exploring new PBM partners within three years. As coverage pools widen, PBMs that master disparate formulary rules, vaccine mandates, and reporting obligations gain scale advantages. Ongoing enrollment growth in India’s Ayushman Bharat and China’s urban employee insurance adds regional tailwinds, enhancing the Pharmacy Benefit Management market outlook.
Shift Toward Value-Based & Outcome-Linked Pharmacy Benefits
Performance-based reimbursement models are moving beyond pilots, with 54% of executives expecting at least a 50% jump in outcome-based contracts by 2025. PBMs apply predictive analytics to risk-stratify members, trigger adherence interventions, and quantify avoided downstream costs. Real-world evidence supplements RCT data in drug evaluations, informing indication-based pricing and shared-savings mechanisms. Transparent metrics improve employer trust and may temper legislative calls for stricter PBM oversight. Value-based designs also encourage manufacturers to back clinical promises with refund or replacement guarantees, reinforcing Pharmacy Benefit Management market innovation.
Digital Transformation & Workflow Automation in PBM Operations
Seventy-seven percent of health leaders rank artificial intelligence as a top technology priority for 2025. Cloud-native claim engines speed prior authorization approvals, flag fraud, and cut average adjudication costs per script. Capital Rx’s Judi Health platform unites medical and pharmacy claims, breaking data silos that inflate total cost of care. Automation frees pharmacists for clinical counseling, raises throughput in mail facilities, and supplies employers near real-time spend dashboards. These advances support the 7.5% CAGR forecast for Claims Processing services and deepen the digital moat of the Pharmacy Benefit Management market.
Restraints Impact Analysis
| Restraints Impact Analysis | (~) % Impact on CAGR Forecast | Geographic Relevance | Impact Timeline |
|---|---|---|---|
| Intensifying legislative & regulatory scrutiny | −1.4% | North America, Europe | Short term (≤ 2 years) |
| Erosion of rebate economics from biosimilar & generic competition | −1.1% | Global | Long term (≥ 4 years) |
| Litigation & margin pressure from independent-pharmacy/DIR reform | −1.0% | North America | Short term (≤ 2 years) |
| Data-privacy & interoperability barriers limiting advanced analytics | −0.8% | Global | Medium term (2-4 years) |
Source: Mordor Intelligence
Intensifying Legislative & Regulatory Scrutiny of PBM Practices
State legislatures introduced 34 targeted PBM bills for the 2025 session, covering spread pricing bans and audit rights. The FTC’s January 2025 interim report claimed the Big Three captured USD 7.3 billion in excess specialty generic markups between 2017 and 2022. Federal proposals, such as the Patients Before Monopolies Act, would separate PBMs from insurer and pharmacy affiliates, raising structural risk for vertically integrated firms. Compliance costs and contract renegotiations may trim margins and slow acquisition pipelines, tempering Pharmacy Benefit Management market expansion in the near term.
Erosion of Rebate Economics from Biosimilar & Generic Competition
Humira biosimilars flooded formularies in 2025, eroding rebate pools that underpinned PBM revenue streams. The gross-to-net gap for branded drugs hit USD 334 billion in 2023 but is narrowing as payers redirect rebates to premium relief. Medicare price-negotiation authority limits rebate leverage on high-spend therapies, while employers push for pass-through models like CVS Health’s CostVantage that surrender 100% of rebates by 2028. PBMs must cultivate alternative revenue—clinical programs, data analytics, and optional administrative fees—reducing reliance on rebates and reshaping long-term Pharmacy Benefit Management market economics.
Segment Analysis
By Service: Claims Processing Drives Digital Transformation
Specialty Pharmacy Services captured 34% of 2024 revenue as complex biologics proliferated in oncology and rare-disease care. Unified care teams, cold-chain logistics, and adherence coaching define this high-touch service line, anchoring the Pharmacy Benefit Management market size leadership among service categories. Claims Processing & Adjudication is projected to grow at 7.5% CAGR to 2030, powered by AI-enabled claim engines that curtail error rates and flag wasteful spending. Capital Rx’s February 2025 launch of Judi Health™ exemplifies the shift to integrated, cloud-native platforms that reconcile medical and pharmacy claims in real time.
Drug Formulary Management continues to pivot from price-tier grids to outcome-centric scorecards that weight real-world evidence and patient-reported metrics. Benefit Plan Design & Consultation helps employers evaluate copay maximizer programs and GLP-1 coverage carve-outs as that class gains weight-management indications. Together, these advisory services supplement transaction-based revenue and support wider adoption of transparent pass-through arrangements across the Pharmacy Benefit Management market.
By Business Model: Government Programs Reshape Market Dynamics
Employer-Sponsored Programs retained 46% market share in 2024, mirroring the central role of job-based insurance in U.S. healthcare. Heightened C-suite focus on drug inflation steers demand toward pass-through pricing, formulary exclusions, and value-based guarantees that limit budget surprises. The Pharmacy Benefit Management market size for Government Health Programs is forecast to advance at a 6.7% CAGR, aided by Medicaid expansion and the out-of-pocket cap in Medicare Part D.
Commercial Health-Insurance Management blends provider-sponsored plans and exchange products, requiring PBMs to synchronize benefit rules across metallic tiers. Direct-to-Consumer Discount-Card Programs proliferate through digital apps that post NADAC-based prices and offer mail-delivery perks. Mark Cuban’s Cost Plus movement underscores consumer appetite for transparent cash pricing, nudging incumbents to modernize benefit designs within the broader Pharmacy Benefit Management market.
By End User: Mail-Order Pharmacies Accelerate Growth
PBM Organizations and Retail Pharmacies together controlled 75.0% of dispensing revenue in 2024, reflecting durable store networks and vertically integrated ownership. The Pharmacy Benefit Management market share of Mail-Order Pharmacies is on track to expand fastest, at an 8.2% CAGR, as home delivery aligns with chronic-care adherence programs and Medicare’s 90-day supply incentives. FTC analysis shows PBM-owned mail pharmacies received reimbursements up to 200-times higher than independents for select oncology products, intensifying policy debate.
Hospital systems pursue specialty-pharmacy accreditation to capture infusion margins and coordinate value-based bundles. Telehealth entrants pair virtual prescribing with automated dispensing centers, widening access and reinforcing the omnichannel direction of the Pharmacy Benefit Management market.
Geography Analysis
North America led with 46.3% of 2024 revenue, anchored by U.S. drug-spend intensity and deep PBM penetration. The region’s oligopolistic PBM triad prompts policy activism, evident in 170 state bills introduced in 2024 to curb spread pricing and clawbacks Bloomberg Law. Inflation Reduction Act provisions that start in 2025 reshape formulary math, prompting contract rewrites and shifting rebate flows within the Pharmacy Benefit Management market.
Asia Pacific registers a 7.6% CAGR outlook, the fastest globally. China alone is projected to hit USD 147.1 billion by 2030 on rising chronic-disease prevalence and policy moves to centralize bulk-drug procurement. India’s growth stems from the Production-Linked Incentive scheme and expansion of Jan Aushadhi generic outlets to 10,500 by March 2025[1]Indian Brand Equity Foundation, “Pharma Companies in India,” ibef.org. Japan’s focus on biopharmaceutical R&D and value-based reimbursement may lift specialty-drug uptake, extending scope for PBM-like services despite demographic headwinds[2]International Society for Pharmaceutical Engineering, “Navigating the Asia Pacific Pharmaceutical Landscape,” ispe.org.
Europe maintains sizable volume under reference-pricing rules and HTA frameworks. Germany’s AMNOG negotiations and the UK’s Voluntary Scheme for Branded Medicines Pricing push PBMs to demonstrate cost-offsets beyond list-price concessions. Middle East & Africa and South America contribute modest shares but display accelerating demand as mandatory health-insurance models roll out. Brazil’s unified procurement of high-cost drugs underscores the region’s appetite for centralized benefit management within the global Pharmacy Benefit Management market.
Competitive Landscape
The Pharmacy Benefit Management market remains highly concentrated: CVS Caremark, Express Scripts, and OptumRx processed about 80% of U.S. claims in 2024. Vertical integration binds these PBMs to insurers and retail or mail pharmacies, bolstering negotiating leverage yet raising conflict-of-interest concerns. The American Medical Association flagged potential anticompetitive risk in markets where the top two PBMs handle 80-90% of scripts[3]American Medical Association, “New AMA Analysis of Consolidation in PBM Markets,” ama-assn.org.
Strategic priorities emphasize scale economics, specialty-drug network control, and data lake investments that fuel predictive adherence interventions. CVS reported that 75% of commercial members adopted two or more features of its TrueCost suite by late 2024, signaling traction for fee-based, pass-through models. Express Scripts advances digital pharmacy channels, while OptumRx integrates behavioral-health datasets to improve medication safety.
Challenger PBMs—Capital Rx, SmithRx, Navitus—win share through transparent network pricing and low fixed fees. Capital Rx’s National Average Drug Acquisition Cost index feeds a clearinghouse model that aligns acquisition costs with client invoices, drawing interest from regional Blues plans. Start-ups test AI-driven prior-auth bots and consumer coupon engines, widening the innovation funnel for the Pharmacy Benefit Management market.
Regulatory scrutiny sharpens competitive risk. The FTC’s January 2025 report could spur structural remedies, while congressional hearings examine mail-pharmacy reimbursement disparities. Incumbents are diversifying into home-infusion, digital therapeutics, and primary-care alignment to offset margin compression, signaling an era of adaptive repositioning.
Pharmacy Benefit Management Industry Leaders
-
Optum Inc.
-
CVS Health (Caremark)
-
Express Scripts (Cigna Evernorth)
-
Humana Pharmacy Solutions
-
Prime Therapeutics LLC
- *Disclaimer: Major Players sorted in no particular order
Recent Industry Developments
- February 2025: Capital Rx launched Judi Health, a unified medical-and-pharmacy claims engine that delivers real-time benefit adjudication and integrated analytics.
- April 2025: Mobile-health Network Solutions agreed to acquire Lifepack, an Indonesian telehealth and pharmacy platform, for up to USD 7.2 million, expanding PBM-adjacent services in Southeast Asia
- March 2024: Prime Therapeutics and Capital Rx formed a strategic alliance to bolster claims-processing efficiency and transparency
Global Pharmacy Benefit Management Market Report Scope
As per the scope of the report, the pharmacy benefit management market plays a significant role in the healthcare industry. It uniquely administers the pharmacy product and focuses on real-time interaction. Pharmacy benefit managers (PBMs) manage prescription drug benefits on behalf of health insurers, Medicare Part D drug plans, large employers, and other payers.
The pharmacy benefit management market is segmented by service, business model, end user, and geography. By service, the market is segmented into specialty pharmacy, drug formulary management, benefit plan design and consultation, and other services. By business model, the market is segmented into government health programs, employer-sponsored programs, and health insurance management. By end user, the market is segmented into pharmacy benefit management organizations, mail-order pharmacies, retail pharmacies, and other end users. By geography, the market is segmented into North America, Europe, Asia-Pacific, the Middle East and Africa, and South America. The report also covers the estimated market sizes and trends for 17 countries across major regions globally. The report offers the value (in USD) for the above segments.
| By Service | Specialty Pharmacy Services | ||
| Drug Formulary Management | |||
| Benefit Plan Design & Consultation | |||
| Other Services | |||
| By Business Model | Government Health Programs | ||
| Employer-Sponsored Programs | |||
| Commercial Health-Insurance Management | |||
| Direct-to-Consumer Discount-Card Programs | |||
| By End User | PBM Organizations (In-house & External) | ||
| Mail-Order Pharmacies | |||
| Retail Pharmacies | |||
| Other End Users | |||
| Geography | North America | United States | |
| Canada | |||
| Mexico | |||
| Europe | Germany | ||
| United Kingdom | |||
| France | |||
| Italy | |||
| Spain | |||
| Rest of Europe | |||
| Asia-Pacific | China | ||
| Japan | |||
| India | |||
| South Korea | |||
| Australia | |||
| Rest of Asia-Pacific | |||
| Middle-East and Africa | GCC | ||
| South Africa | |||
| Rest of Middle East and Africa | |||
| South America | Brazil | ||
| Argentina | |||
| Rest of South America | |||
| Specialty Pharmacy Services |
| Drug Formulary Management |
| Benefit Plan Design & Consultation |
| Other Services |
| Government Health Programs |
| Employer-Sponsored Programs |
| Commercial Health-Insurance Management |
| Direct-to-Consumer Discount-Card Programs |
| PBM Organizations (In-house & External) |
| Mail-Order Pharmacies |
| Retail Pharmacies |
| Other End Users |
| North America | United States |
| Canada | |
| Mexico | |
| Europe | Germany |
| United Kingdom | |
| France | |
| Italy | |
| Spain | |
| Rest of Europe | |
| Asia-Pacific | China |
| Japan | |
| India | |
| South Korea | |
| Australia | |
| Rest of Asia-Pacific | |
| Middle-East and Africa | GCC |
| South Africa | |
| Rest of Middle East and Africa | |
| South America | Brazil |
| Argentina | |
| Rest of South America |
Key Questions Answered in the Report
What is the current size of the Pharmacy Benefit Management market?
The market reached USD 657.51 billion in 2025 and is projected to grow to USD 819.18 billion by 2030 at a 5.6% CAGR.
Why are specialty drugs so important to PBMs?
Specialty medicines represent 54.0% of hospital drug spend in 2025, so payers rely on PBMs for tailored clinical management and price negotiation .
How concentrated is the U.S. PBM sector?
CVS Caremark, Express Scripts, and OptumRx processed about 80% of U.S. prescription claims in 2024
What impact will the Inflation Reduction Act have on PBMs?
Beginning in 2025, Part D out-of-pocket costs are capped at USD 2,000, and price negotiations for selected drugs will alter rebate structures, reshaping PBM revenue models
Which service segment is expanding the fastest?
Claims Processing & Adjudication is forecast to grow 7.5% annually through 2030 as AI platforms streamline real-time decision making
Which region will see the quickest PBM growth?
Asia Pacific is projected to post a 7.6% CAGR, with China alone on track to reach USD 147.1 billion by 2030